Abstract
Objective
Omeprazole, lansoprazole and rabeprazole have been widely used as proton pump inhibitors (PPIs). They can be metabolized in the liver by CYP2C19, a polymorphic enzyme, and have a wide inter-individual variability with respect to drug response. In the investigation reported here, we examined the kinetic characteristics of the three PPIs in healthy Chinese subjects in relation to CYP2C19 genotype status.
Methods
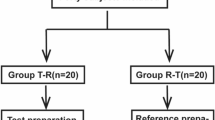
Six homozygous extensive metabolizers (homEMs), six heterozygous extensive metabolizers (hetEMs) and six poor metabolizers (PMs) were recruited for the study from a total of 90 healthy Chinese volunteers whose CYP2C19 genotype status was determined by means of PCR-restriction fragment length polymorphism (RFLP). The study was had an open label, randomized, three-way crossover design. After a single oral dose of 40 mg omeprazole, 30 mg lansoprazole or 40 mg rabeprazole, plasma concentrations of the three PPIs were determined by HPLC.
Results
There were some differences for the area under the plasma concentration-time curve (AUC), the elimination half-life (t1/2ke) and the maximum plasma concentration (cmax) in the three groups. In the homEMs, hetEMs and PMs, the relative AUC0−∞ values were 1:2.8:7.5 for omeprazole, 1:1.7:4.0 for lansoprazole and 1:1.6:3.7 for rabeprazole, respectively; the relative t1/2ke values were 1:1.02:1.65 for omeprazole, 1:1.08:2.39 for lansoprazole and 1:1.37:1.85 for rabeprazole, respectively; the relative cmax values were 1:2.09:4.39 for omeprazole, 1:1.34:1.72 for lansoprazole, and 1:1.24:2.04 for rabeprazole, respectively.
Conclusion
The pharmacokinetic characteristics of the three PPIs are significantly dependent on the CYP2C19 genotype status. These data indicate that individualized dose regimen of the three PPIs, based on identification of genotype, can be of great benefit for ensuring the reasonable use of these drugs.

Similar content being viewed by others
References
Andersson T, Miners JO, Veronese ME, Birkctt DJ (1994) Identification of human liver cytochrome P450 isoforms mediating secondary omeprazole metabolism. Br J Clin Pharmacol 37:597–604
Pichard L, Pedrosa RC, Bonfils C et al (1995) Oxidative metabolism of lansoprazole by human liver cytochromes P450. Mol Pharmacol 47:410–418
VandenBranden M, Ring BJ, Binkley Sn, Wrighton SA (1996) Interaction of human liver cytochromes P450 in vitro with LY307640, a gastric proton pump inhibitor. Pharmacogenetics 6:81–91
Chiba N (1997), Proton pump inhibitors in acute healing and maintenance of erosive or worse esophagitis: a systematic overview. Can J Gastroenterol 11:66B–73B
Kahrilas PJ (2000) Strategies for medical management of reflux disease. Best Pract Res Clin Gastroenterol 14:775–791
Vigneri S, Termini R, Leandro G (1995) comparison of five maintenance therapies for reflux esophagitis. N Engl J Med 333:1106–1110
Dent J, Yeomans ND, Mackinnon M (1994) Omeprazole vs ranitidine for prevention of relapse in reflux oesophagitis. A controlled double blind trial of their efficacy and safety. Gut 35:90–598
Klinkenberg-Knol EC, Festen HP, Jansen JB (1994) Long-term treatment with omeprazole for refractory reflux esophagitis: efficacy and safety. Ann Intern Med 121:161–167
Hu YM, Xu JM, Mei Q, Xu XH, Xu SY (2005) Pharmacodynamic effects and kinetic disposition of rabeprazole in relation to CYP2C19 genotype in healthy Chinese subjects. Acta Pharmacol Sin 26:384–388
Sugimoto M, Furuta T, Shirai N et al. (2004) Different dosage regimens of rabeprazole for nocturnal gastric acid inhibition in relation to cytochrome P450 2C19 genotype status. Clin Pharmacol Ther 76:290–301
Lin CJ, Yang JC, Uang YS, Chern HD, Wang TH (2003) Time-dependent amplified pharmacokinetic and pharmacodynamic responses of rabeprazole in cytochrome P450 2C19 poor metabolizers. Pharmacotherapy 23:711–719
Ieiri I, Kishimoto Y, Okochi H et al ?(2001) Comparison of the kinetic disposition of and serum gastrin change by lansoprazole versus rabeprazole during an 8-day dosing scheme in relation to CYP2C19 polymorphism. Eur J Clin Pharmacol 57:485–492
Shu Y, Zhou HH (2000) Individual and ethnic differences in CYP2C19 activity in Chinese populations. Acta Pharmacol Sin 21:193–199
Bertilsson L, Lou YQ, Du YL et al (1992) Pronounced differences between native Chinese and Swedish populations in the polymorphic hydroxylations of deb risoquin and S-mephenytoin. Clin Pharmacol Ther 51:388–397
Edeki TI, Goldstein JA, de Morais SMF et al (1996) Genetic polymorphism of S-mephenytoin 4’-hydroxylation in African-Americans. Pharmacogenetics 6:357–360
de Morais SMF, Wilkinson GR, Blaisdell J (1994) The major genetic defect responsible for the polymorphism of S–mephenytoin metabolism in humans. J Biol Chem 269:15419–15422
de Morais SMF, Wilkinson GR, Blaisdell J, Meyer UA, Nakamura K, Goldstein JA (1994) Identification of a new genetic defect responsible for the polymorphism of (S)-mephenytoin metabolism in Japanese. Mol Pharmacol 46:594–598
Ieri I, Kubota T, Urae A et al (1996) Pharmacokinetics of omeprazole (a substrate of CYP2C19) and comparison with two mutant alleles, C gamma P2C19m1 in exon 5 and C gamma P2C19m2 in exon 4, in Japanese subjects. Clin Pharmacol Ther 59:647–653
Tanigawara Y, Aoyama N, Kita T et al (1999) CYP2C19 genotype-related efficacy of omeprazole for the treatment of infection caused by Helicobacter pylori. Clin Pharmacol Ther 66:528–534
Ando T, Kato H, Sugimoto N et al (2005) A comparative study on endoscopic ulcer healing of omeprazole versus rabeprazole with respect to CYP2C19 genotypic differences. Dig Dis Sci 50:1625–1631
Itagaki F, Homma M, Yuzawa K et al (2004) Effect of lansoprazole and rabeprazole on tacrolimus pharmacokinetics in healthy volunteers with CYP2C19 mutations. J Pharm Pharmacol 56:1055–1059
Lee SB, Park SJ, Ryu JK et al (2003) Efficacy of triple therapy with rabeprazole for Helicobacter pylori infection in relation to CYP2C19 genotype. KorJ Gastroenterol 42:468–475
Goldstein JA, Blaisdell J (1996) Genetic tests which identify the principal defects in CYP2C19 responsible for the polymorphism in mephenytoin metabolism. In: Johnson EF, Waterman MR (ed) Methods in enzymology, vol 272: cytochrome P450. Academic, New York pp 210–218
Yuen KH, Choy WP, Tan HY (2001) Improved high performance liquid chromatographic analysis of omeprazole in human plasma. J Pharm Biomed Anal 2001:715–720
Karol MD, Granneman GR, Alexander K (1995) Determination of lansoprazole and five metabolites in plasma by high-performance liquid chromatography. J Chromatogr B 668:182–186
Asuda S, Ohnishi A, Ogawa T et al (1994) Pharmacokinetic properties of E3810, a new proton pump inhibitor, in healthy male volunteers. Int J Clin Pharmacol Ther 32:466–471
Furuta T, Shirai N, Sugimoto M, Ohashi K, Ishizaki T (2004) Pharmacogenomics of proton pump inhibitors. Pharmacogenomics 5:181–202
Evans WE, Relling MV (2004) Moving towards individualized medicine with pharmacogenomics. Nature 429:464–468
Meyer UA (2004) Pharmacogenetics – five decades of therapeutic lessons from genetic diversity. Nat Rev Genet 5:669–676
Yasuda S, Horai Y, Tomono Y et al (1995) Comparison of the kinetic disposition and metabolism of E3810, a new proton pump inhibitor, and omeprazole in relation to S-mephenytoin 4´-hydroxylation status. Clin Pharmacol Ther 58:143–154
Sugimoto M, Furuta T, Shirai N et al. (2005) Comparison of an increased dosage regimen of rabeprazole versus a concomitant dosage regimen of famotidine with rabeprazole for nocturnal gastric acid inhibition in relation to cytochrome P450 2C19 genotypes. Clin Pharmacol Ther 77:302–311
Horn J (2004) Review article: relationship between the metabolism and efficacy of proton pump inhibitors – focus on rabeprazole. Aliment Pharmacol Ther 20:11–19
Furuta T, Shirai N, Xiao F, Ohashi K, Ishizaki T (2001) Effect of high-dose lansoprazole on intragastic pH in subjects who are homozygous extensive metabolizers of cytochrome P4502C19. Clin Pharmacol Ther 70:484–492
Acknowledgements
We thank the volunteers for their participation in this study. This study was supported by the Engineering Project for Innovative Scholars of Henan Province. The experiments comply with the current laws of the country in which they were performed, inclusive of the approval of the Ethics Committee.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qiao, HL., Hu, YR., Tian, X. et al. Pharmacokinetics of three proton pump inhibitors in Chinese subjects in relation to the CYP2C19 genotype. Eur J Clin Pharmacol 62, 107–112 (2006). https://doi.org/10.1007/s00228-005-0063-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-005-0063-1