Abstract
Objective:
The goal of this study was to describe the changes in plasma creatinine levels that occur in prematurely born neonates, to better understand the use of the terms ‘renal dysfunction’ and ‘renal failure’ among premature neonates, as well as to evaluate the demographic and outcome characteristics associated with renal problems in preterm neonates who have no major congenital anomalies.
Study Design:
Retrospective review of the Pediatrix neonatal intensive care patient clinical data warehouse.
Result:
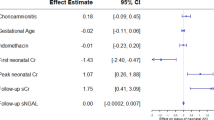
The study cohort consisted of neonates born with an estimated gestational age of ⩽30 completed weeks in whom there was no report of any major anomalies (n=66 526). In this group of 66 526 neonates, there were 64 030 (96.2%) with no report of renal dysfunction or failure, 1239 (1.9%) in whom there was a diagnosis of renal dysfunction and 1257 infants (1.9%) with a diagnosis of renal failure. The clinical circumstances most strongly associated with a diagnosis of renal dysfunction and/or renal failures were low gestational age and birth weight. In addition, multivariate analysis showed that the factors associated with an increased risk of renal problems were vasopressor use during the first 7 days after birth, grade 3 or 4 intraventricular hemorrhage, a patent ductus arteriosus, necrotizing enterocolitis, male gender, the use of indomethacin, a positive blood culture during the first 7 days after birth, the use of high-frequency ventilation in the first 2 days after birth, non-White race and prolonged exposure to antibiotics. Mortality was higher in patients with renal problems than in neonates without renal problems (39.1 vs 10.2%, P<0.01) and higher in neonates with renal failure than in neonates with renal dysfunction (57.6 vs 20.1%, P<0.01).
Conclusion:
Renal dysfunction and/or failure are common diagnoses, especially in extremely premature neonates and there are potentially modifiable factors that increase the risk of renal problems.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Iacobelli S, Bonsante F, Ferdinus C, Labenne M, Gouyon JB . Factors affecting postnatal changes in serum creatinine in preterm infants with gestational age <32 weeks. J Perinatol 2009; 29: 232–236.
Thayyil S, Sheik S, Kempley ST, Sinha A . A gestational age and postnatal age-based reference chart for assessing renal function in extremely premature infants. J Perinatol 2008; 28: 226–229.
Cuzzolin L, Fanos V, Pinna B, di Marzio M, Perin M, Tramontozzi P et al. Postnatal renal function in preterm newborns: a role of diseases, drugs and therapeutic interventions. Pediatr Nephrol 2006; 21: 931–938.
Mathur NB, Agarwal HS, Maria A . Acute renal failure in neonatal sepsis. Indian J Pediatr 2006; 73: 499–502.
Cataldi L, Leone R, Moretti U, De MB, Fanos V, Ruggeri L et al. Potential risk factors for the development of acute renal failure in preterm newborn infants: a case-control study. Arch Dis Child Fetal Neonatal Ed 2005; 90: F514–F519.
Chevalier RL, Campbell F, Brenbridge AN . Prognostic factors in neonatal acute renal failure. Pediatrics 1984; 74: 265–272.
Stapleton FB, Jones DP, Green RS . Acute renal failure in neonates: incidence, etiology and outcome. Pediatr Nephrol 1987; 1: 314–320.
Choker G, Gouyon JB . Diagnosis of acute renal failure in very preterm infants. Biol Neonate 2004; 86: 212–216.
Guignard JP, Drukker A . Why do newborn infants have a high plasma creatinine? Pediatrics 1999; 103: e49.
Miall LS, Henderson MJ, Turner AJ, Brownlee KG, Brocklebank JT, Newell SJ et al. Plasma creatinine rises dramatically in the first 48 hours of life in preterm infants. Pediatrics 1999; 104: e76.
Singh BS, Clark RH, Powers RJ, Spitzer AR . Meconium aspiration syndrome remains a significant problem in the NICU: outcomes and treatment patterns in term neonates admitted for intensive care during a ten-year period. J Perinatol 2009; 29 (7): 497–503.
Laughon M, Bose C, Clark R . Treatment strategies to prevent or close a patent ductus arteriosus in preterm infants and outcomes. J Perinatol 2007; 27: 164–170.
Garges HP, Moody MA, Cotten CM, Smith PB, Tiffany KF, Lenfestey R et al. Neonatal meningitis: what is the correlation among cerebrospinal fluid cultures, blood cultures, and cerebrospinal fluid parameters? Pediatrics 2006; 117: 1094–1100.
Clark RH, Chace DH, Spitzer AR . Effects of two different doses of amino acid supplementation on growth and blood amino acid levels in premature neonates admitted to the neonatal intensive care unit: a randomized, controlled trial. Pediatrics 2007; 120: 1286–1296.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Journal of Perinatology website
Supplementary information
Rights and permissions
About this article
Cite this article
Walker, M., Clark, R. & Spitzer, A. Elevation in plasma creatinine and renal failure in premature neonates without major anomalies: terminology, occurrence and factors associated with increased risk. J Perinatol 31, 199–205 (2011). https://doi.org/10.1038/jp.2010.82
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2010.82
Keywords
This article is cited by
-
Congenital anomalies of the kidney and urinary tract (CAKUT) in critically ill infants: a multicenter cohort study
Pediatric Nephrology (2023)
-
Neonatal acute kidney injury risk stratification score: STARZ study
Pediatric Research (2022)
-
Creatinine filtration kinetics in critically Ill neonates
Pediatric Research (2021)
-
Clinical outcomes of hypertensive disorders in pregnancy in the offspring during perinatal period, childhood, and adolescence
Journal of Human Hypertension (2021)
-
Assessment of Vancomycin Pharmacokinetics and Dose Regimen Optimisation in Preterm Neonates
Drugs in R&D (2020)