Abstract
Objective
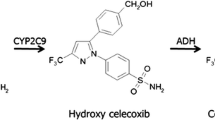
To analyse the influence of age and cytochrome P450 (CYP) 2C9 genotype on the steady-state disposition of the standard NSAID diclofenac and the new COX-2 selective inhibitor celecoxib, both of which are metabolised by the polymorphically expressed CYP2C9.
Design
Double-blind randomised crossover study under steady-state conditions.
Subjects
12 young (age 32 ± 5 years, bodyweight 71 ± 12kg; mean ± SD) and 12 elderly (68 ± 2 years, 82 ± 15kg) healthy, drug-free, nonsmoking Caucasians of both sexes.
Methods
All subjects received oral celecoxib (200mg twice daily) and diclofenac (75mg twice daily) for 15 days separated by a drug-free interval of at least 3 weeks. Following the last morning dose, multiple blood samples were taken for 25 hours. Concentrations of celecoxib and diclofenac were measured by specific and sensitive high performance liquid chromatography. Identification of CYP2C9 genotype was performed by genomic DNA sequencing. Pharmacokinetic parameters for total and unbound drugs were individually analysed by noncompartmental techniques.
Results
For diclofenac, area under the concentration-time curve over the dosage interval (AUC τ) was larger in young subjects (3.2 ± 1.0 mg · h/L) than in older individuals (2.4 ± 0.4 mg · h/L; p < 0.05). As the terminal half-life (t½z) was very similar in both groups (3.9 ± 4.4 vs 3.5 ± 3.3 hours), either less complete absorption in the elderly or their higher bodyweight could account for the difference. For celecoxib, AUCτ (5.8 ± 1.7 vs 5.6 ± 2.3 mg · h/L) and t½z (11.8 ± 8.7 vs 11.2 ± 2.9 hours) were almost identical in young and older subjects. Plasma protein binding of both NSAIDs was unaffected by age, and apparent oral clearances for unbound drugs were not different between the two groups of healthy subjects. When considering the genotype of all individuals (CYP2C9*1/*1, n = 10; CYP2C9*1/*2, n = 6; CYP2C9*2/*2, n = 2; CYP2C9*1/*3, n = 4; CYP2C9*3/*3, n = 1), no association with any pharmacokinetic parameter of either drug was apparent. Moreover, there was no significant correlation between the AUC values of celecoxib and diclofenac.
Conclusions
Age and CYP2C9 genotype do not significantly affect the steady-state disposition of celecoxib and diclofenac. This would indicate that both drugs need no dosage reduction in the elderly (at least up to 75 years) and that, besides CYP2C9, additional CYP species contribute to the elimination of both agents.





Similar content being viewed by others
References
Thomson AH, Tucker GT. Gerontokinetics: a reappraisal. Br J Clin Pharmacol 1992; 33: 1–2
Avorn J. Including elderly people in clinical trials. BMJ 1997; 315: 1033–4
Greengross S, Murphy E, Quam L, et al. Aging: a subject that must be at the top of world agendas. BMJ 1997; 315: 1029–30
Winker MA. Aging: a global issue [letter]. JAMA 1997; 278: 1377
Parker BM, Cusack BJ, Vestal RE. Pharmacokinetic optimisation of drug therapy in elderly patients. Drugs Aging 1995; 7: 10–8
Kinirons MT, Crome P. Clinical pharmacokinetic considerations in the elderly: an update. Clin Pharmacokinet 1997; 33: 302–12
Hughes SG. Prescribing for the elderly patient: why do we need to exercise caution? Br J Clin Pharmacol 1998; 46: 531–3
Turnheim K. Drug dosage in the elderly: is it rational? Drugs Aging 1998; 13: 357–79
Le Couteur DG, McLean AJ. The aging liver: drug clearance and an oxygen diffusion barrier hypothesis. Clin Pharmacokinet 1998; 34: 359–73
Hämmerlein A, Derendorf H, Lowenthal DT. Pharmacokinetic and pharmacodynamic changes in the elderly: clinical implications. Clin Pharmacokinet 1998; 35: 49–64
Herrlinger C, Klotz U. Drug metabolism and drug interactions in the elderly. Best Pract Res Clin Gastroenterol 2001; 15: 897–918
Davies NM, Anderson KE. Clinical pharmacokinetics of diclofenac: therapeutic insights and pitfalls. Clin Pharmacokinet 1997; 33: 184–213
Woodhouse KW, Wynne H. The pharmacokinetics of non-steroidal anti-inflammatory drugs in the elderly. Clin Pharmacokinet 1987; 12: 111–22
Jackson LM, Hawkey CJ. COX-2 selective nonsteroidal antiinflammatory drugs: do they really offer any advantages? Drugs 2000; 59: 1207–16
FitzGerald GA, Patrono C. The coxibs, selective inhibitors of cyclooxygenase-2. N Engl J Med 2001; 345: 433–42
Davies NM, McLachlan AJ, Day RO, et al. Clinical pharmacokinetics and pharmacodynamics of celecoxib: a selective cyclo-oxygenase-2 inhibitor. Clin Pharmacokinet 2000; 38: 225–42
Clemett D, Goa KL. Celecoxib: a review of its use in osteoarthritis, rheumatoid arthritis and acute pain. Drugs 2000; 59: 957–80
Paulson SK, Hribar JD, Liu NW, et al. Metabolism and excretion of [14C]celecoxib in healthy male volunteers. Drug Metab Dispos 2000; 28: 308–14
Leemann T, Transon C, Dayer P. Cytochrome P450TB (CYP2C): a major monooxygenase catalyzing diclofenac 4″-hydroxylation in human liver. Life Sci 1993; 52: 29–34
Tang C, Shou M, Mei Q, et al. Major role of human liver microsomal cytochrome P450 2C9 (CYP2C9) in the oxidative metabolism of celecoxib, a novel cyclooxygenase-II inhibitor. J Pharmacol Exp Ther 2000; 293: 453–9
Shimamoto J, Ieiri I, Urae A, et al. Lack of differences in diclofenac (a substrate for CYP2C9) pharmacokinetics in healthy volunteers with respect to the single CYP2C9*3 allele. Eur J Clin Pharmacol 2000; 56: 65–8
Morin S, Loriot MA, Poirier JM, et al. Is diclofenac a valuable CYP2C9 probe in humans? Eur J Clin Pharmacol 2001; 56: 793–7
Tang C, Shou M, Rushmore TH, et al. In-vitro metabolism of celecoxib, a cyclooxygenase-2 inhibitor, by allelic variant forms of human liver microsomal cytochrome P450 2C9: correlation with CYP2C9 genotype and in-vivo pharmacokinet-ics. Pharmacogenetics 2001; 11: 223–35
Schönberger F, Heinkele G, Mürdter TE, et al. Simple method for the determination of celecoxib in human serum by HPLC with fluorescence detection. J Chromatogr B Analyt Technol Biomed Life Sci 2002; 768: 255–60
Bradford MM. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-binding. Anal Biochem 1976; 72: 248–54
Wang S, Huang J, Lai MD, et al. Detection of CYP2C9 polymorphism based on the polymerase chain reaction. Pharmacogenetics 1995; 5: 37–42
Sullivan-Klose TH, Ghanayem BI, Bell DA, et al. The role of the CYP2C9-Leu359 allelic variant in the tolbutamide polymorphism. Pharmacogenetics 1996; 6: 341–9
Tanswell P, Heinzel G, Weisenberger H, et al. Pharmacokinetic-pharmacodynamic and metabolite modeling with TopFit. Int J Clin Pharmacol Ther 1995; 33: 550–4
Haslock I. Clinical economics review: gastrointestinal complications of non-steroidal anti-inflammatory drugs. Aliment Pharmacol Ther 1998; 12: 127–33
Lichtenberger LM. Where is the evidence that cyclooxygenase inhibition is the primary cause of nonsteroidal anti-inflammatory drug (NSAID)-induced gastrointestinal injury? Topical injury revisited. Biochem Pharmacol 2001; 61: 631–7
Eras J, Perazella MA. NSAIDs and the kidney revisited: are selective cyclooxygenase-2 inhibitors safe? Am J Med Sci 2001; 321: 181–90
Pacifici GM, Viani A. Methods of determining plasma and tissue binding of drugs: pharmacokinetic consequences. Clin Pharmacokinet 1992; 23: 449–68
Paulson SK, Kaprak TA, Gresk CJ, et al. Plasma protein binding of celecoxib in mice, rat, rabbit, dog and human. Biopharm Drug Dispos 1999; 20: 293–9
Schall R, Hundt HKL, Luus HG. Pharmacokinetic characteristics of absorption and clearance in drug/drug interaction studies. Int J Clin Pharmacol Ther 1994; 32: 633–7
Streetman DS, Bertino JS Jr, Nafziger AN. Phenotyping of drug-metabolizing enzymes in adults: a review of in-vivo cytochrome P450 phenotyping probes. Pharmacogenetics 2000; 10: 187–216
Tanaka E. In vivo age-related changes in hepatic drug-oxidizing capacity in humans. J Clin Pharm Ther 1998; 23: 247–55
Loebstein R, Yonath H, Peleg D, et al. Interindividual variability in sensitivity to warfarin: nature or nurture? Clin Pharmacol Ther 2001; 70: 159–64
Stubbins MJ, Harries LW, Smith G, et al. Genetic analysis of the human cytochrome P450 CYP2C9 locus. Pharmacogenetics 1996; 6: 429–39
Scordo MG, Pengo V, Spina E, et al. Influence of CYP2C9 and CYP2 C19 genetic polymorphisms on warfarin maintenance dose and metabolic clearance. Clin Pharmacol Ther 2002; 72: 702–10
García-Martín E, Martínez C, Ladero JM, et al. High frequency of mutations related to impaired CYP2C9 metabolism in a Caucasian population. Eur J Clin Pharmacol 2001; 57: 47–9
Yasar Ü, Eliasson E, Dahl ML, et al. Validation of methods for CYP2C9 genotyping: frequencies of mutant alleles in a Swedish population. Biochem Biophys Res Commun 1999; 254: 628–31
Aynacioglu AS, Brockmöller J, Bauer S, et al. Frequency of cytochrome P450 CYP2C9 variants in a Turkish population and functional relevance for phenytoin. Br J Clin Pharmacol 1999; 48: 409–15
Scordo MG, Aklillu E, Yasar U, et al. Genetic polymorphism of cytochrome P450 2C9 in a Caucasian and a black African population. Br J Clin Pharmacol 2001; 52: 447–50
Yoon YR, Shon JH, Kim MK, et al. Frequency of cytochrome P450 2C9 mutant alleles in a Korean population. Br J Clin Pharmacol 2001; 51: 277–80
Martin JH, Begg EJ, Kennedy MA, et al. Is cytochrome P450 2C9 genotype associated with NSAID gastric ulceration? Br J Clin Pharmacol 2001; 51: 627–30
Yasar Ü, Eliasson E, Forslund C, et al. Metabolism of losartan and diclofenac by polymorphic CYP2C9 [abstract]. Drug Metab Rev 2001; 33 Suppl. 1: 225
Yasar Ü, Eliasson E, Forslund-Bergengren C, et al. The role of CYP2C9 genotype in the metabolism of diclofenac in vivo and in vitro. Eur J Clin Pharmacol 2001; 57: 729–35
Chen M-L, Lesko L, Williams RL. Measures of exposure versus measures of rate and extent of absorption. Clin Pharmacokinet 2001; 40: 565–72
Acknowledgements
The study was supported by the Robert Bosch Foundation, Stuttgart, Germany. We greatly appreciate the valuable support of Dr E. Schäffeler with the genotyping and Dr T. Ray (Novartis, East Hanover, NJ, USA) for the generous gift of purified [14C]diclofenac. There are no potential conflicts of interest directly relevant to the content of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brenner, S.S., Herrlinger, C., Dilger, K. et al. Influence of Age and Cytochrome P450 2C9 Genotype on the Steady-State Disposition of Diclofenac and Celecoxib. Clin Pharmacokinet 42, 283–292 (2003). https://doi.org/10.2165/00003088-200342030-00003
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003088-200342030-00003